Project Leader: Andrew Liu, MD
Project Personnel: Allison Schiltz
Background
Recently, a U.S.-wide survey linked household endotoxin exposure to asthma, making it a U.S. public health concern. However, it is not known whether ambient endotoxin exerts its pathogenic effects on asthma persistence, severity and/or causation.
Hypothesis
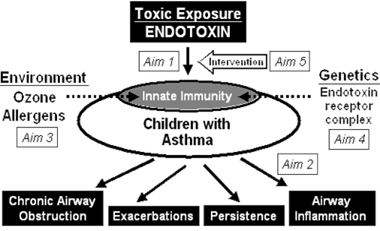
We hypothesize that higher levels of endotoxin exposure cause persistent, problematic asthma and that key environmental (ozone and allergens) and genetic modifiers (endotoxin receptor polymorphisms) contribute to endotoxin susceptibility and pathological asthmatic responses. We propose to study these endotoxin-induced airway conditions in children through three complementary clinical investigations.
Specific Aims
First, we will conduct an ancillary study of a NIH-sponsored multicenter cohort of children with asthma (Childhood Asthma Management Program), which has tracked asthma severity for over a decade, to determine if endotoxin exposure, modified by genetics and environment, is associated with greater disease severity and persistence.
Second, we will conduct a panel study of children with asthma to investigate whether endotoxin exposure, modified by environment, is associated with inflamed airways and elevated TLR expression on airway macrophages. Clinically, these inflammatory responses could drive poor asthma control and exacerbations.
Finally, we will collaborate with a HUD-sponsored inner-city home intervention study to determine if a home environment intervention will reduce home endotoxin levels and improve asthma.
This combination of studies will provide an understanding of how endotoxin interacts with other potentially toxic exposures in the susceptible host to cause persistent, problematic asthma. These studies will help us to determine the levels of endotoxin exposure that are likely to be problematic for children with asthma, and to develop environmental educational and intervention programs to improve outcomes.